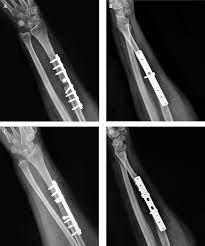
Bone grafts are procedures that replace or rebuild bone that is missing or weakened due to injury, disease or surgery. When bone is damaged, it needs to be repaired to regain its full function and provide structure and support to the body. Bone grafts rely on the body’s natural bone healing process. Bone can be replaced or rebuilt using bone grafts taken from the patient’s own body or using substitutes derived from natural or synthetic sources. The demand for bone grafts and substitutes is rising across Latin America and this article provides an overview of these products and procedures in the region.
Autografts – The Gold Standard
An autograft refers to using a patient’s own bone for grafting purposes. This involves surgically removing bone from a non-weight-bearing area of the patient’s skeleton and implanting it at the site requiring reconstruction. Autografts are considered the gold standard for bone grafts as it eliminates disease transmission risks and has the best graft incorporation and healing success rates. However, autograft procedures also have disadvantages like requiring a secondary surgery at the donor site which risks infection and limited donor bone availability. Nevertheless, autografts remain the most widely used bone grafting option currently in Latin America due to its superior results.
Allografts – Using Donor Bone
An allograft involves using bone tissue harvested from a cadaveric donor. The donor bone is carefully processed to eliminate disease transmission risks while preserving the natural structure and bone-forming cellular activity. Common sources include femoral heads, cortical bone strips/wedges, cancellous chips and demineralized bone matrices. Allografts provide an of-the-shelf alternative to autografts while avoiding donor site morbidity. However, Bone Graft and Substitutes also carry a higher risk of immune rejection compared to autografts. Stringent donor screening and tissue processing help improve allograft safety and they are becoming increasingly common bone graft substitutes across Latin American countries.
Demineralized Bone Matrices – The Cellular Toolkit
Demineralized bone matrices or DBMs are processed allografts that have been further deproteinized to remove antigenic properties and immunogenicity. This leaves behind the collagen matrix and bone morphogenetic proteins (BMPs) that provide the cellular toolkit for new bone formation. DBMs stimulate the activity of osteoprogenitor cells present at the graft site, facilitating regeneration. They are usually combined with other grafting materials to act as a natural bone graft extender or substitute. DBMs provide an acellular off-the-shelf option suitable even for immunocompromised patients. Their use is gaining prominence across orthopedic and dental procedures in Latin America.
Synthetic Bone Grafts – The Manufactured Alternatives
Synthetic bone grafts are human-made alternatives that include calcium phosphate ceramics, bioactive glass and polymer composites. Calcium phosphates like hydroxyapatite and beta-tricalcium phosphate are extensively used as they can be naturally resorbed and replaced by new bone over time. Their porous structure allows for new bone ingrowth. Bioactive glass reacts with body fluids to form a carbonated hydroxyapatite layer that bonds to living bone. Synthetic grafts eliminate disease risks associated with allografts and their composition can be tailored as per application. While synthetic grafts do not promote natural osteoinduction like allografts, continuous product innovation is improving their bone regeneration capacities. They act as viable graft substitutes, especially for low-risk, non-load-bearing indications across Latin America.
Bone Morphogenetic Proteins – Nature’s Osteoinductors
Bone morphogenetic proteins (BMPs) are growth factors naturally found in the human body that play a key role in bone and cartilage formation during the process of ossification. Purified recombinant human BMPs like rhBMP-2 and rhBMP-7 are now being extensively used as components of bone grafting products to enhance new bone formation. When implanted at orthopedic and dental defect sites, they induce migration and differentiation of mesenchymal stem cells into osteoblasts. rhBMPs therefore provide the essential osteoinductive cues missing from synthetic or allograft bone substitutes. Their inclusion in grafting solutions is helping drive enhanced bone healing outcomes across Latin America. However, highdose rhBMP use also faces concerns regarding rare ectopic or soft tissue bone formation.
Cell-Based Bone Regeneration
Advancements in tissue engineering are now enabling development of cell-based bone graft substitutes. These involve seeding osteoprogenitor or stem cells onto 3D scaffolds made from natural or synthetic polymers to create living grafts. The scaffold provides an osteoconductive surface for cell attachment, proliferation and new bone matrix deposition. Sources of cells being explored include autologous or allogeneic BMSCs, adipose-derived stem cells or platelet-rich plasma derivatives. Some cell-seeded scaffold devices are exhibiting promising results in small animal and clinical studies. While cell-based grafts face challenges regarding donor availability, standardization and high manufacturing costs currently, they represent the future of customized bone regeneration solutions tailored for specific patient needs across Latin America.
*Note:
1. Source: Coherent Market Insights, Public sources, Desk research
2. We have leveraged AI tools to mine information and compile it