Diabetes management has come a long way in recent years with revolutionary technological advancements. One such advancement that has transformed diabetes care is continuous glucose monitoring (CGM) devices. These devices provide real-time glucose readings throughout the day and night without the need for finger pricks.
What is Continuous Glucose Monitoring?
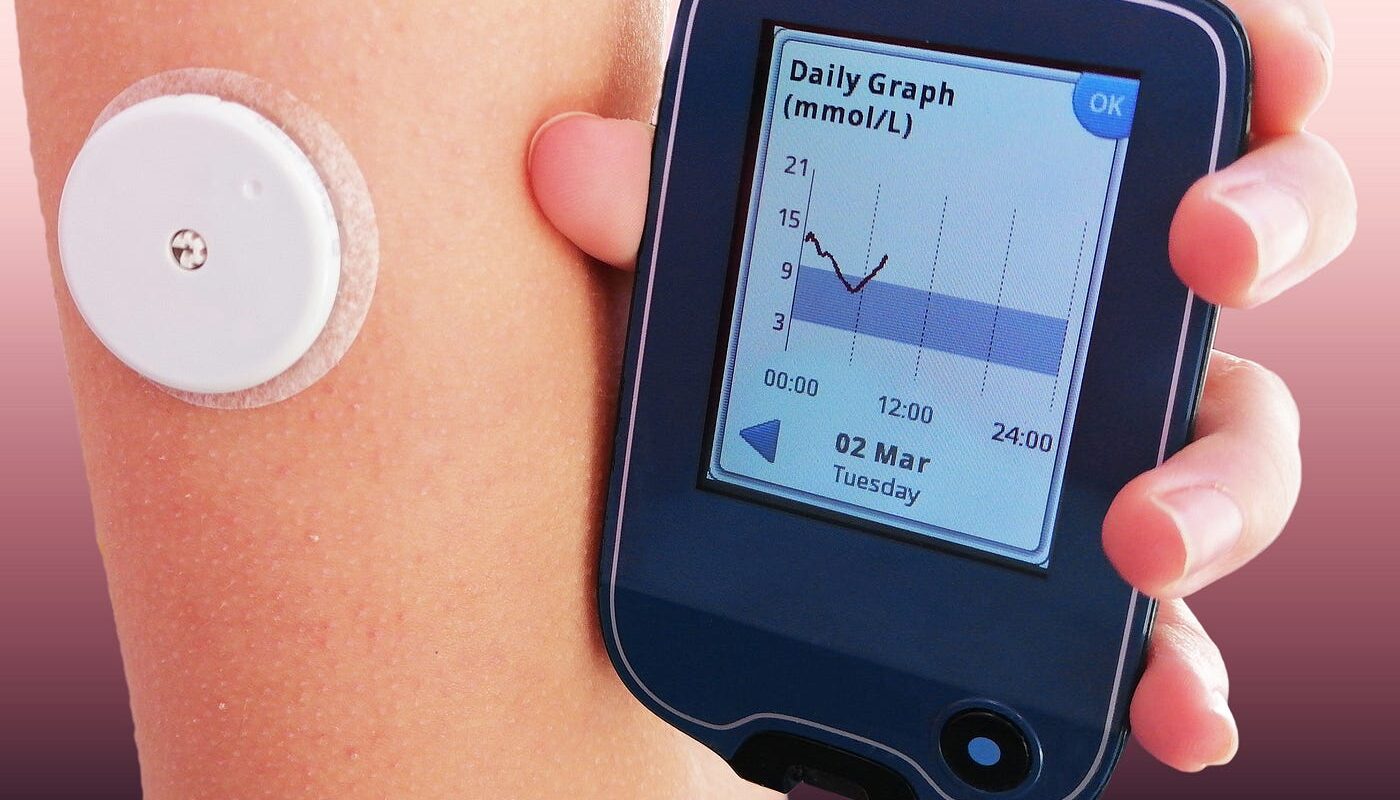
Continuous glucose monitoring uses a tiny sensor inserted under the skin, usually on the belly or arm, to check glucose levels in interstitial fluid. The sensor measures glucose every few minutes and sends readings wirelessly to a receiver or smartphone. This allows individuals to regularly monitor trends in their glucose levels without having to draw blood through finger pricks.
There are two main types of CGM systems available – real-time and retrospective. Real-time Continuous Glucose Monitoring Devices display current glucose readings, trends, and alerts right on a dedicated receiver or smartphone. This type provides readings every 1 to 5 minutes. Retrospective or flash CGMs still require scanning with a reader but provide readings for the past 8 hours without displaying current levels. Both system types are factory calibrated and do not require calibration with blood glucose meters.
Benefits of Continuous Glucose Monitoring
CGM offers numerous benefits compared to fingerstick blood glucose monitoring alone. Some of the key benefits include:
– Improved Glucose Control: Studies have found CGM use leads to significant reduction in A1c levels, indicating better long-term glucose control. This is due to more frequent readings allowing faster adjustments.
– Detection of Trends: CGM sensors can detect subtle rises and falls in glucose levels between fingerstick checks. This allows individuals to proactively respond to changing trends.
– Reduced Hypos and Hypers: Real-time alerts for low and high glucose help manage hypos and hypers more effectively to avoid complications.
– Peace of Mind: Not having to prick fingers multiple times a day reduces pain and stress. CGM provides constant reassurance about glucose levels throughout the day and night.
– Enhanced Lifestyle Flexibility: CGM empowers individuals to exercise more freedom in daily routines like mealtimes and activities while still maintaining optimal control.
– Improved Decision Making: Healthcare providers can use detailed CGM reports to optimize medication dosage, carb ratios, and make treatment adjustments.
Using Continuous Glucose Monitoring
Here are a few key points about using CGM devices:
Insertion and Wear: CGM sensors are inserted under the skin, similar to an insulin pump insertion set. Sensors are changed every 7-14 days depending on the device. The small insertion site is usually on the belly or back of the upper arm.
Calibration: While factory calibrated, some CGM systems may require fingerstick calibration a few times a day. Retrospective devices do not require calibration.
Alerts: Real-time CGM devices have customizable alarms to warn of impending highs and lows so action can be taken. Thresholds can be set to each individual’s needs.
Patterns and Trends: By viewing glucose graphs over time, patterns emerge which provide valuable insights on how activity, diet, and medications impact levels throughout the day and night.
Sharing Data: Data from some devices can be shared remotely with loved ones or care teams using smartphone apps. This facilitates team management of diabetes.
The Future of Continuous Glucose Monitoring
Research into CGM technology continues at a rapid pace. Exciting advancements on the horizon include:
– Artificial Pancreas Systems: Combining insulin pumps and high-accuracy CGM to automatically adjust insulin based on glucose readings with minimal input from the user.
– Longer Wear Sensors: Sensors lasting 14-30 days in development to further improve convenience and reduce insertion sites over time.
– Non-Invasive Monitoring: Transdermal sensor technologies are in trials to detect glucose through the skin or other methods eliminating the need for sensor insertion.
– Wider Accessibility: As technologies mature and costs decrease, CGM is becoming affordable and accessible for more individuals living with diabetes. Goal is mainstream adoption.
*Note:
1. Source: Coherent Market Insights, Public sources, Desk research
2. We have leveraged AI tools to mine information and compile it