Compartment syndrome refers to a painful condition where pressure builds within the compartments of the body, compromising circulation and potentially causing permanent damage. It can occur due to trauma such as fractures or crush injuries, or post-surgery. Left untreated, compartment syndrome leads to chronic disability or even amputation.
For centuries, doctors have relied solely on clinical examination such as checking pain and swelling levels to detect compartment syndrome risk. However, these techniques often miss the condition until it is too late to reverse damage. In the past decade, medical technology has advanced tremendously with the development of compartment syndrome monitoring devices that can continuously and objectively measure tissue pressure in at-risk limbs. These new devices are revolutionizing compartment syndrome diagnosis and treatment globally.
How Compartment Syndrome Monitoring Devices Work
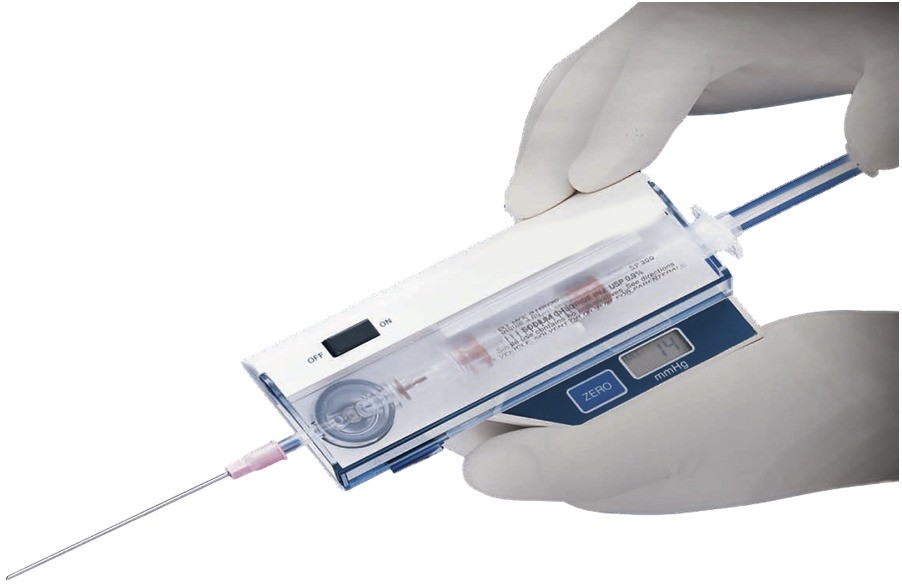
Compartment Syndrome Monitoring Devices typically involve a small, flexible probe inserted into the tissue compartment of concern, connected to a monitor via cables. The probe contains a pressure transducer that measures and wirelessly transmits interstitial fluid pressure readings in near real-time to the monitor.
Devices can provide pressures every few seconds to minutes continuously for hours or days depending on the model. Pressure thresholds are set by doctors based on clinical risk factors, and alerts are generated if pressure rises above the threshold. This objectively confirms the diagnosis of compartment syndrome that may otherwise have gone undiagnosed until severe harm occurred.
Impact on Patient Outcomes
Early detection through monitoring allows timely fasciotomy – surgical release of compartment pressures before permanent tissue injury sets in. Studies show monitoring significantly reduces amputation rates, from over 70% without monitoring to around 5% when compartment pressures are objectively measured.
Less invasive fasciotomy and fewer amputations translate to marked improvements in functional recovery and quality of life for patients. Furthermore, monitoring prevents many unnecessary fasciotomies by distinguishing compartment syndrome from harmless swelling based solely on pressures. This spares patients from invasive surgery when not required.
Uptake in Clinical Settings
While still not widely used in all regions globally, compartment syndrome monitoring adoption is accelerating. Factors driving uptake include strong clinical evidence, lower device costs, and better reimbursement recognition by insurers of the technology’s clear benefits.
Orthopedic trauma centers on the frontlines of limb-threatening injuries have been early adopters. General surgical floors and emergency departments are also incorporating monitors into protocols for at-risk patients like those with multiple long bone fractures or crush injuries. With education and experience, monitoring is becoming routine practice in high-risk scenarios.
Military surgeons have likewise recognized compartment syndrome’s disproportionate impact on combat casualties, where extremity trauma is common. Deployed monitors allow earlier fasciotomy and decreased medical evacuations – significant advantages in resource-constrained warzones. Most modern militaries now include monitoring in standard of care guidelines for wounded soldiers.
Ongoing Development and New Frontiers
Continual innovation aims to expand application and value of compartment syndrome monitoring. Smaller, lower-cost devices enable broader clinical and even pre-hospital use cases. Non-invasive sensors under investigation could eliminate probe insertion risks. Wireless platforms enable full mobility during monitoring.
Data integration capabilities link monitors to electronic health records for complete pressure documentation. Connected platforms allow remote monitoring by offsite surgeons. Artificial intelligence analytics of pressure tracings may one day provide automated diagnostic insights.
Emerging applications range from post-traumatic limb salvage to monitoring reconstructive flap or replant viability. Some explore using similar techniques to track intracranial pressure dynamics. As compartment syndrome understanding grows, monitoring use will likely extend to new anatomical sites and non-trauma conditions with compartment concerns, like reperfusion injury.
Conclusion
Compartment syndrome monitoring represents a remarkable triumph of medical technology improving patient outcomes. By continuously measuring tissue pressures objectively, these devices empower clinicians to make sound diagnoses and ensure the best chances of limb salvage through timely intervention. As costs fall and adoption expands, monitoring promises to benefit many more compromised limbs globally each year. Continued innovation will only strengthen this revolution inmusculoskeletal care.
*Note:
1. Source: CoherentMI, Public sources, Desk research
2. We have leveraged AI tools to mine information and compile it